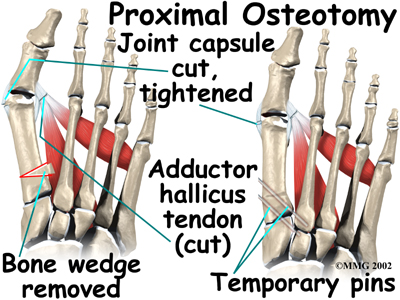
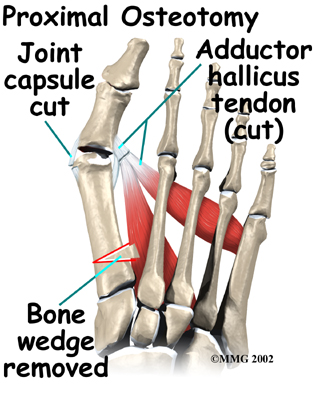
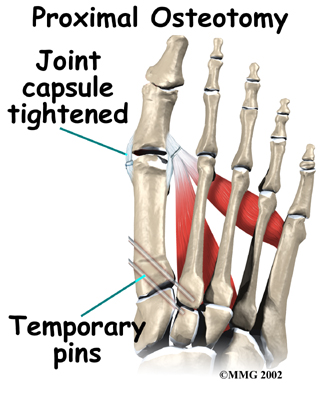
What can be done for the condition?
Nonsurgical Rehabilitation
Our Physical Therapists & Occupational Therapists at PhysioPartners can assist you in many ways with a painful bunion and hallux valgus. Treatment of hallux valgus nearly always starts with adapting footwear to fit the foot. Your Physical Therapist & Occupational Therapist will ask you many questions about the type of shoes you wear and may even ask you to bring your shoes in so we can observe them. In the early stages of hallux valgus, converting from a shoe with a pointed toe to a shoe with a wide forefoot (or toe box) may arrest the progression of the deformity. Since the pain that arises from the bunion is due to pressure from the shoe, treatment focuses on removing the pressure that the shoe exerts on the deformity and wider shoes immediately reduce the pressure on the bunion and the added space in this part of the shoe keeps the metatarsals from getting squeezed. Bunion pads may also reduce pressure and rubbing from the shoe. Your Physical Therapist & Occupational Therapist will advise you on the best shoes for your condition. There are also numerous devices, such as toe spacers, that attempt to splint the big toe and reverse the deforming forces. Many of these spacers are designed to be worn during the night but a few can be worn during the day in a shoe with a larger shoe box. Special bunion pads are also available that are placed over the bunion to relieve some of the direct pressure.Your Physical Therapist & Occupational Therapist will discuss whether these devices would be useful for you and inform you on where you can purchase them. Taping can be trialled as a cheaper alternative and can help you decide if a rigid support may help. In addition, your Physical Therapist & Occupational Therapist may suggest the use of foot orthotics depending on the alignment of your arch. The orthotics support the arch and hold the big toe in better alignment.
When the bunion is acutely painful the above changes to your footwear and use of splints may allow you to resume normal walking immediately, but it is still wise to cut back on more vigorous activities for several weeks to allow the inflammation and pain to subside. Your Physical Therapist & Occupational Therapist can advise you, however, on alternative activities that allow you to maintain your cardiovascular fitness while you allow the pain in your toe to settle. A stationary bicycle, rowing machine, or water activities like running or aerobics are good alternatives to activities such as regular running or walking.
Physical Therapy & Occupational Therapy treatment at PhysioPartners can also assist with decreasing the pain and swelling caused by the bunion.
Your Physical Therapist & Occupational Therapist may use electrical modalities such as ultrasound or interferential current to reduce your pain. Moist heat or ice may also be recommended as a pain-reliever. A more hands-on treatment such as soft-tissue massage around the area or mobilizations of the joints of the toe and foot may also be used by your Physical Therapist & Occupational Therapist. These mobilizations help to gently stretch the tissues and encourage the joints to move into their normal range of motion. Therapy sessions sometimes include iontophoresis, which uses a mild electrical current to push anti-inflammatory medicine to the sore area.
In addition to assisting with the pain and swelling, your Physical Therapist & Occupational Therapist may prescribe some simple stretching and strengthening exercises for the foot and toe to combat the progression of the deformity. Exercises to strengthen the muscles that lift your arch may also be prescribed.
Lastly, your Physical Therapist & Occupational Therapist will assess the alignment and entire biomechanics of your lower limbs while you stand still and while you walk. If you are a runner, they may also ask you to bring your runners and assess your running biomechanics. Abnormal alignment or biomechanics can lead to poor use of the foot and added pressure onto an already painful bunion. Once we have assessed your entire lower limb, we may prescribe strengthening or stretching exercises for areas that to you seem unrelated to your foot, such as your hip, knee or core area. These areas, however, are particularly important in maintaining the alignment and posture through your leg and into your foot and toe.
Although the Physical Therapy & Occupational Therapy treatment we offer at PhysioPartners often provides significant relief from a painful bunion, if you continue to experience significant pain or the problem seems to be getting worse, a surgical consult may be required.
PhysioPartners provides services for Physical Therapy & Occupational Therapy in Chicago.
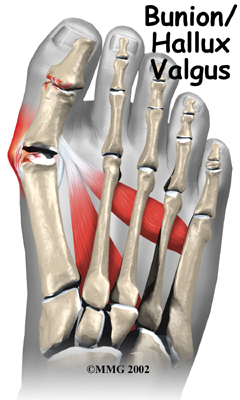

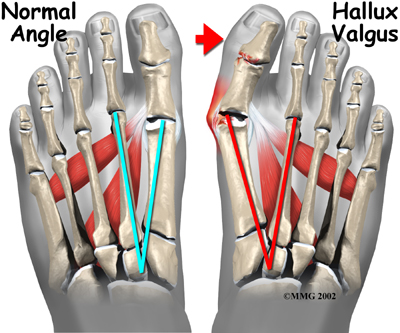
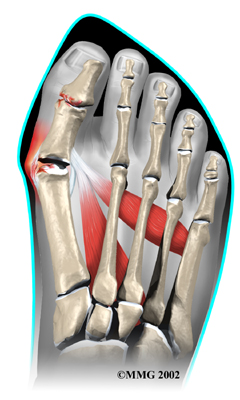
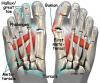 One of the other changes that occurs is that the bone just above the big toe, the first metatarsal, usually develops too much of an angle in the other direction. This condition is called metatarsus primus varus. Metatarsus primus means first metatarsal, and varus is the medical term that means the deformity goes in a direction towards the midline of the body. This creates a situation where the first metatarsal and the big toe now form an angle with the point sticking out at the inside edge of the ball of the foot. The bunion that develops is actually a response to the pressure from the shoe on the point of this angle. At first the bump is made up of irritated, swollen tissue that is constantly caught between the shoe and the bone beneath the skin. As time goes on, the constant pressure may cause the bone to thicken as well, creating an even larger lump to rub against the shoe.
One of the other changes that occurs is that the bone just above the big toe, the first metatarsal, usually develops too much of an angle in the other direction. This condition is called metatarsus primus varus. Metatarsus primus means first metatarsal, and varus is the medical term that means the deformity goes in a direction towards the midline of the body. This creates a situation where the first metatarsal and the big toe now form an angle with the point sticking out at the inside edge of the ball of the foot. The bunion that develops is actually a response to the pressure from the shoe on the point of this angle. At first the bump is made up of irritated, swollen tissue that is constantly caught between the shoe and the bone beneath the skin. As time goes on, the constant pressure may cause the bone to thicken as well, creating an even larger lump to rub against the shoe.